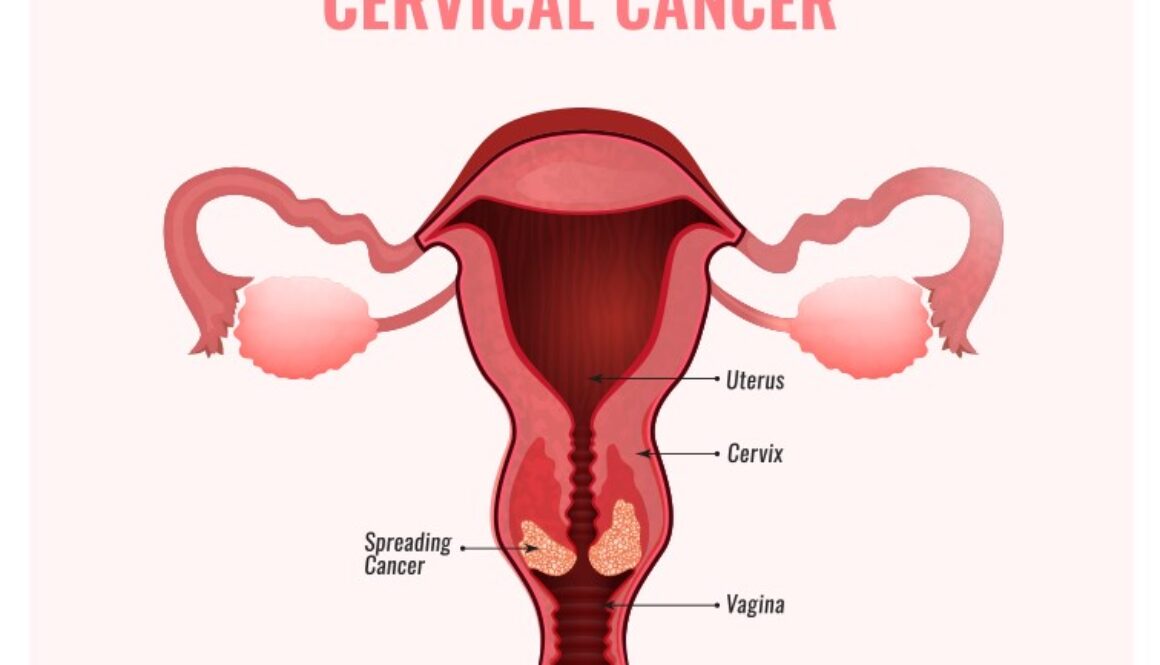
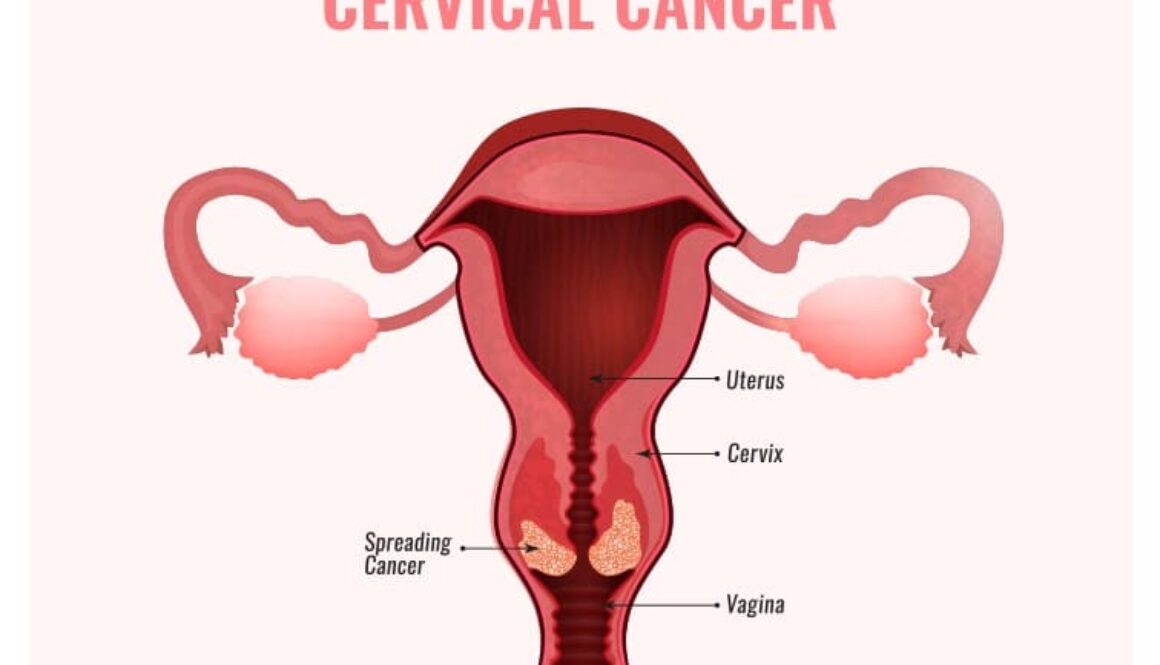
Stage IV cervical Cancer: Symptoms & Treatment
Cervical cancer, though highly preventable with regular screenings and HPV vaccinations, remains a significant health concern globally. When diagnosed early, cervical cancer treatment is quite promising. In addition, stage IV cervical cancer treatment options are evolving as active research in this area is flourishing. However, in cases where the cancer progresses to Stage IV, the challenges intensify. Stage IV cervical cancer indicates that the cancer has spread beyond the cervix to nearby tissues and organs or distant parts of the body. Let us try to understand more about the symptoms, diagnosis, and options for Stage IV cervical cancer treatment.
Cervical Cancer Symptoms
The symptoms of Stage IV cervical cancer can vary depending on the extent of the cancer’s spread. However, common signs may include:
- Pelvic Pain: Pain in the pelvic area, lower back, or throughout the pelvic region can occur as the cancer progresses.
- Urinary Symptoms: This may include frequent urination, blood in the urine, or difficulty urinating, as the cancer may affect the bladder or kidneys.
- Bowel Symptoms: Changes in bowel habits, such as constipation or blood in the stool, may occur if cancer spreads to the rectum or colon.
- Swelling: Swelling in the legs or other areas of the body may develop due to lymph node involvement or obstruction of blood flow.
- Weight Loss: Unexplained weight loss can occur
- Fatigue: Persistent fatigue can be a symptom of advanced cervical cancer, as the body works to combat the disease.
- Bone Pain: if the cancer spreads to the bones, it may cause pain or fractures.
- Shortness of Breath: If the cancer spreads to the lungs, it can lead to difficulty breathing.
Other symptoms include – spitting blood, bone pain or fractures, and irregular bleeding.
Diagnosis
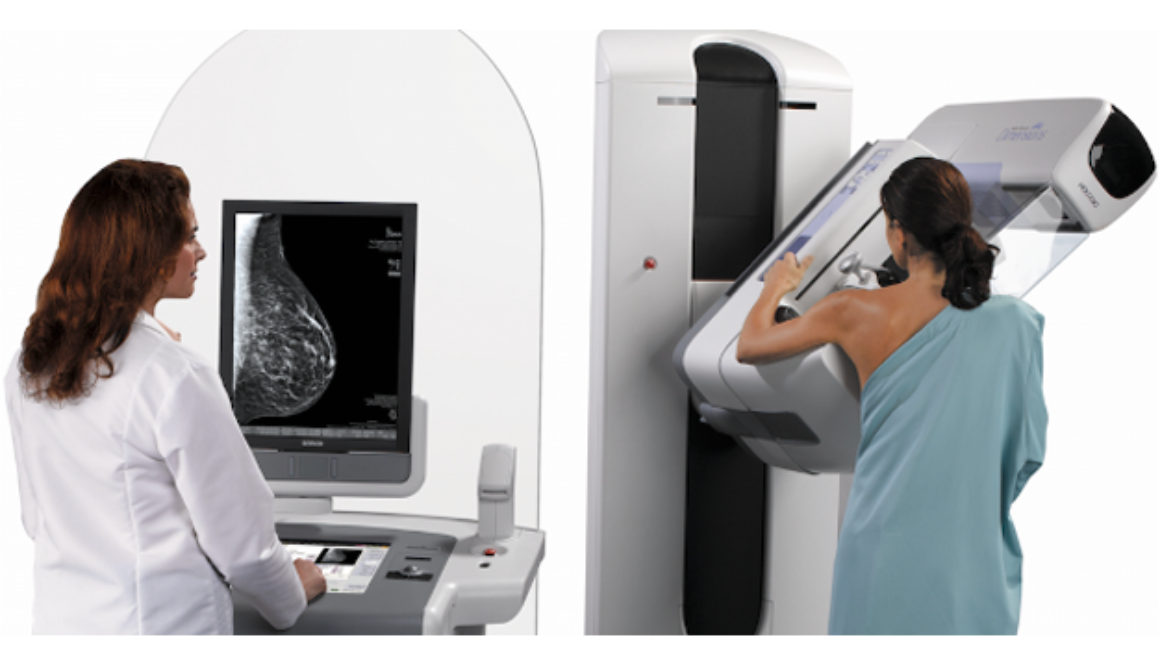
Diagnosing Stage IV cervical cancer typically involves a combination of imaging tests, such as CT scans, MRIs, or PET scans, to determine the extent of the cancer’s spread. Additionally, a biopsy may be performed to confirm the presence of cancer cells and to assess their characteristics, which can help guide treatment decisions.
Stage 4 means the cancer has spread outside the cervix and uterus to the following areas:
- The cancer has spread to the lining of the rectum
- The cancer has spread to the lining of the bladder
- Outside the area between the hip bones (pelvis)
- Cervical cancer has spread to the lungs
Stage IV Cervical Cancer Treatment
Treatment for Stage IV cervical cancer is often complex and may involve a combination of approaches aimed at controlling the cancer, relieving symptoms, and improving quality of life.
Treatment depends on the location of the cancer, the type of cancer, and other health conditions the person may have. The stage of cancer may also help the doctor decide the type of treatment.
Treatment options for stage IV cervical cancer may include:
- Chemotherapy: Chemotherapy uses powerful drugs to kill cancer cells or stop them from growing. It is often used as a primary treatment for Stage IV cervical cancer or in combination with other therapies.
- Radiation Therapy: Radiation therapy uses high-energy rays to target and destroy cancer cells. It may be used alone or in combination with chemotherapy, particularly for cancers that have spread to nearby tissues or organs. Both external and internal radiotherapy is given.
- Surgery: In some cases, surgery may be recommended to remove cancerous tumors or to alleviate symptoms, such as pain or blockages.
- 4. Targeted Therapy: Targeted therapy drugs are designed to specifically target cancer cells while minimizing damage to healthy cells. These drugs may be used in combination with other treatments for Stage IV cervical cancer.
- Immunotherapy: Immunotherapy works by harnessing the body’s immune system to recognize and attack cancer cells. It is an area of active research for cervical cancer treatment, particularly in advanced stages.
- Palliative Care: Palliative care focuses on providing relief from symptoms and improving the quality of life for patients with advanced cancer. It may include pain management, emotional support, and assistance with practical aspects of care. In addition to all the possible options for stage IV cervical cancer treatment, palliative care is indispensable.