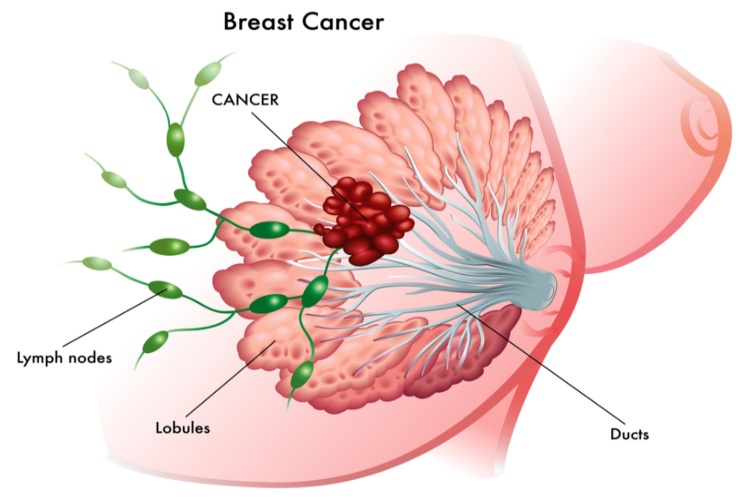
Breast conservation Surgery – What You Need to Know? Oncoplastic breast conservation surgery performed by an experienced and expert breast surgeon leads to lower re-excision rates compared to standard breast conservation surgery (therapy). With this type of surgery, the surgeon performs extensive resection without compromising breast aesthetics. An excellent surgical outcome with respect to oncoplastic breast conservation surgery for breast cancer requires – the experience, expertise and dexterity of the female breast oncoplastic surgeon. In addition to the technical skills and overall experience of performing complex breast surgeries – the breast oncoplastic surgeon’s other attributes – such as the number of surgeries performed in the past (repetitive ability of performing breast conservation surgeries with precision); dedication of the surgeon and decision-making skills are also indispensable. A Modern, Experienced Lady Oncoplastic Surgeon Must Follow some Specific and Crucial Steps – including the following: Ultrasonography, mammography and Magnetic Imaging-guided local staging of the cancer. Comprehensive preoperative study of the tumour with respect to calcifications and localization. Selection of the best oncoplastic breast surgical technique based on the decision taken collectively by a multidisciplinary surgery board. Selection of surgical technique tailormade according to the patient’s needs. Intraoperative ultrasound-guided resection of the tumour. Intraoperative radiological and pathological evaluation of the tumour for defining the lesion and margins of resection. Defining tumour bed within the excision cavity to guide adjuvant breast radiotherapy. The above parameters will help in improving both the oncological and cosmetic outcomes of the procedure – keeping the breast aesthetics intact as the excision of healthy breast tissue is kept minimum. Bottom Line Oncoplastic breast conservation surgery is being increasingly used with exceptional outcomes as the technique helps in extensive resection of breast tissue with safer margins – improving breast aesthetics. Therefore, breast cancer patients who require surgery should consider this option. Breast-conserving surgery is sometimes called lumpectomy, quadrantectomy, partial mastectomy, or segmental mastectomy depending on how much tissue is removed. To know more about breast conservation oncoplastic surgery – meet me personally for a one-to-one discussion. Dr Geetha Nagasree Breast Oncoplastic Surgeon Call – 9908216809 Read More – TYPES OF BREAST CANCER SURGERIES TYPES OF BREAST CANCER Heal, Therapy, Insight Facebook Twitter Linkedin
Laparoscopic Surgery for Uterine Fibroids Removal
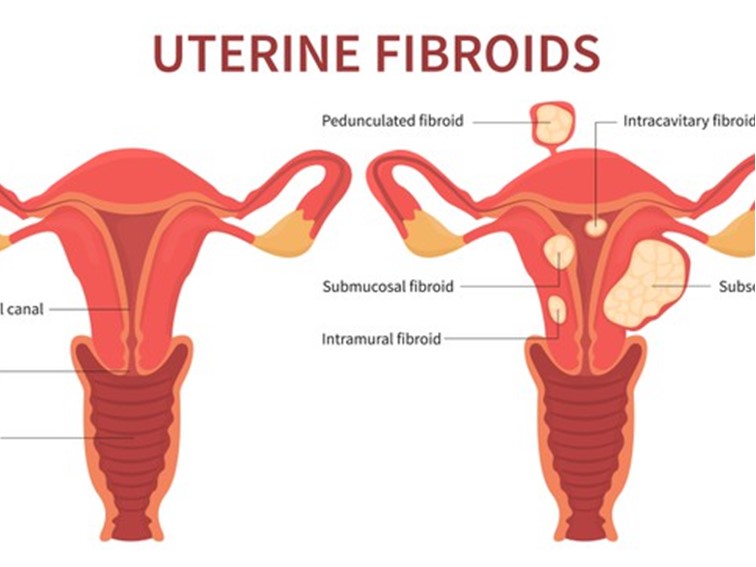
Laparoscopic myomectomy: Uterine fibroids are the common noncancerous growths that develop in the uterus most commonly during childbearing years, but can also occur at any age. Prior to going into details about laparoscopic myomectomy in Hyderabad, let us understand, why you need this type of surgery. A majority of women of reproductive age and between 30 to 45 years of age have uterine fibroids. They can be completely asymptomatic or can cause abnormally heavy and prolonged menstruation, urinary problems, abdominal pressure, dyspareunia, and pelvic pain. However, the signs and symptoms of fibroids depend on the size and location in the uterus. Prominent symptoms The most prominent symptom associated with uterine fibroid is Abnormal bleeding – especially when the fibroids are adjacent to the uterine cavity. The severity of symptoms, to a large extent, depends on the size of fibroids. Smaller fibroids cause fewer symptoms or no symptoms (completely asymptomatic). In general, fibroids are non-malignant as less than 1% may turn malignant. Symptoms of Uterine Fibroids Pelvic pressure and pain Abdominal discomfort Prolonged or heavy periods Bleeding between periods Difficulty getting pregnant Pain during intercourse Low back pain Frequent urination Key facts about Fibroids A routine pelvic exam helps in detecting uterine Fibroids. These are the most common non-malignant (benign growths) of the reproductive tract (uterus) in women. About 80% of women may develop uterine fibroids at some point during their lifetime. Prolonged periods, heavy periods, bleeding in between periods, pelvic pressure, and pain are the most common symptoms of uterine fibroids. The symptoms associated with fibroids depend on their size and location in the uterus. Women approaching menopause are at higher risk. The treatment approaches depend on the size, location, and the objective of preserving fertility Myomectomy Myomectomy is a surgical procedure that removes only the fibroids leaving the uterus – whereas hysterectomy removes the entire uterus. The goal of the gynecologist who specializes in laparoscopic myomectomy is to remove fibroids and reconstruct the uterus. Laparoscopic myomectomy in Hyderabad Laparoscopic fibroid removal surgery is a minimally invasive procedure for the removal of uterine fibroids from the uterus. In this procedure, three to four small incisions are made in the abdomen, and then small, tube-like specialized surgical instruments are inserted through these incisions into the abdomen. A laparoscope is a small, narrow tube-like instrument with a camera. It helps in guiding the surgeon in performing surgery. The fibroids are cut and removed. The benefits of laparoscopic myomectomy include less scarring, minimal blood loss, less pain, shorter hospital stay, fewer complications, and faster recovery and return to normal activities. Why It is Done? Symptoms associated with fibroids are problematic and interfere with daily activities. They also interfere with your fertility. Your gynaecologist will prefer laparoscopic myomectomy instead of hysterectomy if surgery is recommended for uterine fibroids. She will prefer this type of surgical approach to preserve your fertility because you are planning to have children and don’t want to remove your uterus. Bottom Line Laparoscopic myomectomy helps in relieving recurrent and nagging symptoms – such as pelvic pain, pressure and heavy bleeding, and other symptoms associated with uterine fibroids. If you have these symptoms – and unsure of where to go for a laparoscopic myomectomy in Hyderabad, then meet me.
Rare Types of Breast Cancer & Their Treatment
Rare types of breast cancer: Around 70% of breast cancers are an invasive type of carcinomas. Oncologists have developed several ways of grouping breast cancers into different types. The rare types of breast cancers are known as “SPECIAL TYPE” whereas more common ones are termed as “NO SPECIAL TYPE” Lymphoma of the Breast These are a rare type of breast cancers as they make up only 1% or less in as many as 100 cases of breast cancer. Among the non-Hodgkin lymphomas (NHL) the most common types include extranodal marginal zone lymphomas and B-cell lymphomas. Peripheral T-cell lymphoma is a less common type. Breast implant-associated anaplastic large cell lymphoma (BIA-ALCL) is another rare type of NHL. It rarely develops in women who have breast implants. Seroma or swelling around the implant is the first sign, and some women may also develop a lump close to the implant. The symptoms may manifest sooner or later after breast implant surgery. If it is localized (which is otherwise called in situ), the implant is removed and no further treatment is usually needed. However, in some cases, oncologists prescribe medicines to treat it. The outlook is good. However, in infiltrative type (i-ALCL), a lump can be felt in the breast and cancer may spread to the lymph nodes as well. A breast oncoplastic surgeon removes the implant and the lymph nodes and also prescribe chemotherapy and radiotherapy. Metaplastic Breast Cancer This type is a heterogeneous group of invasive and aggressive breast cancer. This type of breast cancer is also very rare (less than 5%) and is common in black and Hispanic women. It usually occurs in middle-aged and older women (age 50 to 60 years and above). The treatment is the same – surgery, chemotherapy and radiotherapy. Though these cancers do not spread to the lymph nodes, they are more likely to spread to other body parts. Sometimes, these cancers are triple-negative as well. Adenoid Cystic Carcinoma of the Breast It is a slow-growing cribriform cancer – which is less than 1% (which means, 1 in 100 breast cancer cases are adenoid cystic cancer). Cancer develops in the breast tissue and most often diagnosed in the salivary glands. It is common in older people, but can also be seen in young women. Surgery is the best option – breast conservation surgery (lumpectomy) is performed. This type of cancer rarely spread to other parts of the body. The recurrence rate is quite low – and hence the outlook is excellent. Tubular Breast Cancer This type of breast cancer looks like tubes under a microscope – and hence, it is known as tubular type. It is a very rare type of cancer (less than 2%). Tubular cancer can spread to nearby lymph nodes. It is commonly detected in older women. The recurrence rate is low as it doesn’t come back after treatment. The outlook is therefore excellent. Mucinous (Mucoid or Colloid) Breast Cancer This rare type of breast cancer occurs very rarely (1 to 2%). The name mucinous is due to the large amount of mucin it has. Sometimes, it can be a mixture of mucinous and other types. The treatment is the same as with any other type – breast surgery (mastectomy or lumpectomy), chemotherapy and radiation therapy. It is slow-growing cancer usually detected in older women. It doesn’t spread to lymph nodes. Oncologists may recommend sentinel node biopsy to see whether cancer has spread to the lymph nodes. Mucinous carcinoma of the breast – colloid carcinoma (abnormal cells of the tumour float in pools of mucin (a slimy and slippery component of mucus). Accounts for 2 to 3% of breast cancers. Less aggressive type as it responds well to treatment. The outlook for mucinous breast cancer is generally very good. Medullary carcinoma of the breast It is a rare type of breast cancer accounting for up to 1 – 5% of breast cancers. It occurs most commonly in younger women – especially those who have faulty BRCA 1 gene. Oncologists and pathologist identify these types of tumours by looking at the cell boundaries of cancer cells that clearly separate tumour cells from normal tissues. The tumour cells also contain white blood cells. The medullary tumour appears like a soft, fleshy mass – low grade and less aggressive in nature and easy to treat. The treatment is the same as for other types of invasive breast cancers – surgery, medication, radiation therapy. The outlook is good. Basal Type Breast Cancer In this type of breast cancer, genetic changes are unique – owing to which cancer cells make large amounts of cytokeratin 5/6 protein. Hormone and targeted drug therapies don’t work with this type as mostly these types of cancers are triple-negative (They lack the receptors for HER2, Progesterone and Oestrogen). Therefore, the treatment modalities usually involve surgery, chemotherapy and radiation therapy. Learn more about other rare types of breast cancer
Breast Cancer Treatment – Types of Surgeries & Therapies
Breast cancer behaviour and biology affect the treatment. Some types of breast cancers are aggressive – though they are small, they grow quickly.
What You Need to Know About Ovarian Cysts full Information
What You Need to Know About Ovarian Cysts full Information The best lady doctor for ovarian cysts in Hyderabad comprehensively explains everything about ovarian cysts What You Need to Know About Ovarian Cysts | Dr Geetha Nagasree Ovarian Cysts Types, Symptoms, Causes and Diagnosis Dr. Geetha Nagasree is the best lady doctor for ovarian cyst in Hyderabad. According to her, every woman must know about ovarian cysts, their risks, types of cysts, symptoms, and the diagnosis of ovarian cysts. Ovaries constitute a part of the female reproductive system. They are located on either side of the uterus in the lower abdomen. Two ovaries produce eggs as well as estrogen and progesterone hormones. Cysts are fluid-filled sacs or solid pockets that develop on one or both ovaries. Cysts are common in women, and in the majority of cases, they cause no symptoms. They go away on their own. They become problematic when they persist and become bigger. Cysts can cause pain. Though there is no possibility of a cyst developing into cancer, the risk is there. The risk of a cyst developing into ovarian cancer is rare but increases with age. Ovarian cysts in women after menopause are more likely to be cancerous than those in younger women. Types of ovarian cysts Ovarian cysts are of different types—such as dermoid cysts, cystadenomas, endometriomas, follicle cysts, and corpus luteum cysts. Follicle cysts and corpus luteum cysts are functional cysts (they are part of the monthly cycle). Follicle cyst An egg grows inside a sac within the ovary. This sac is known as a follicle. The sack breaks open and releases an egg. If the sac doesn’t break open, a cyst develops within the follicle. This type of cyst may last for a month or two and then go away on its own. Corpus luteum cysts The sac of the follicle usually dissolves after it releases an egg. Sometimes the sac doesn’t dissolve (shrink), and further fluid accumulates in it. The opening then seals, and the fluid inside it causes a corpus luteum cyst to develop. This type of cyst may go away in a few weeks. Similarly, cystadenomas are cysts that develop on the outer surface of the ovaries,, and dermoid cysts are sac-like growths on the ovaries. In some women, a large number of cysts develop on their ovaries. This condition is known as polycystic ovarian syndrome (PCOS). It can cause infertility if left untreated. Risk factors for ovarian cysts Hormonal abnormalities, drugs that induce fertility, a severe pelvic infection, endometriosis, and a personal history of ovarian cysts can increase the risk of developing ovarian cysts. Symptoms of Ovarian Cysts Ovarian cysts usually cause no symptoms. The symptoms may manifest as the cyst grows and include the following: Abdominal pain Sharp or dull pain on one side of the belly Bloating or swelling Painful bowel movements Nausea and vomiting Pelvic pain Fever, sharp or intense pelvic pain, dizziness, faintness, and rapid breathing are the symptoms associated with ovarian trouble and warrant immediate medical attention. Call for emergency help straight away if you experience these symptoms. Complications associated with ovarian cysts Ovarian cysts usually don’t cause any severe complications, as they are mostly benign and go away on their own. On rare occasions, during routine medical check-ups and gynecological examinations, your gynecologist may notice a cystic ovarian mass, which could be cancerous. Another rare complication of an ovarian cyst is ovarian torsion. In this case, a large cyst displaces the ovary from its position, due to which the ovary twists and moves away. The twisting of the ovary may result in the breakdown of the blood supply to it causing ovarian tissue damage and death. Though ovarian torsion is very rare, it is an emergency medical condition. Approximately 3 to 4% of women on average undergo emergency gynecologic surgeries due to this condition. Ovarian cysts, sometimes, rupture and cause severe pain and internal bleeding. Though ruptured cysts are rare, the condition causes intense pain and increases the risk of life-threatening infection. Diagnosis of Ovarian Cyst A gynecologist performs a physical examination, including a routine pelvic examination, to inspect female reproductive organs. Based on the medical history of the patient and existing symptoms, your gynecologist may recommend a pelvic examination once or twice a year. The diagnostic tests that your gynecologist orders to diagnose ovarian cysts include pelvic ultrasound, blood test, laparoscopy, and the CA 125 blood test (the levels of this protein are elevated in a woman with ovarian cancer). An abdominal CT scan may also be recommended to detect ovarian cysts. Read: The Treatment for Ovarian Cyst Dr Geetha Nagasree The best lady doctor for ovarian cyst in Hyderabad Heal, Therapy, Insight Facebook Twitter Linkedin
Endometrial Uterine Cancer Causes Risk Factors & Symptoms
Endometrial (Uterine) Cancer – Causes, Risk Factors & Symptoms Uterus is a hollow, pear-shaped organ in which fetal development occurs The uterus is a hollow, pear-shaped organ in which fetal development occurs. A layer of cells forms the lining (endometrium) of the uterus or womb. Cancerous cells grow in the endometrium and cause endometrial cancer. Thus, endometrial cancer begins in the uterus. Endometrial cancer is also known as Uterine Cancer. Causes of Uterine Cancer Endometrial cancer risk factors: The exact cause of endometrial cancer is unknown. However, the risk increases with advancing age, strong family history, and genetic mutations. Alterations in the gene sequence within the endometrial cells lining the uterus can cause uterine cancer. Genetic mutations turn healthy and normal cells into abnormal cells, which grow and multiply at an abnormal rate. The abnormal cells accumulate and form a mass (tumour). Cancerous cells spread aggressively by invading nearby healthy tissues and then spreading to other organs of the body (metastasize). Signs and Symptoms of Uterine Cancer What are Endometrial cancer Risk factors? Hormonal imbalances – especially the changes in the levels of two main female hormones: estrogen and progesterone – produced by the ovaries can cause changes in the endometrium. A health condition that augments the levels of estrogen hormone, but not progesterone can raise the risk. Such conditions include diabetes, obesity, and polycystic ovarian syndrome. Post-menopausal hormonal therapy involving estrogen hormones can also increase cancer risk. A type of ovarian cancer that increases the levels of estrogen hormone can increase the risk of uterine cancer. Hormone therapy for breast cancer increases the risk of getting endometrial cancer. However, the drug tamoxifen prescribed for the treatment of breast cancer outweighs the small risk of uterine cancer. Therefore, those who are taking tamoxifen should discuss the risk with their doctor. Endometrial Cancer Risk Factors – Age The risk of endometrial cancer increases with age – older women who have undergone menopause are at increased risk. The risk of endometrial cancer increases in women who started menstruation at an early age and undergone menopause at a later age. Women who have never been pregnant are at risk of developing endometrial cancer. How to Reduce the Risk of Endometrial Cancer? Physical activity and regular exercise may reduce the risk of endometrial cancer. Women age over 40 years should seriously consider a daily exercise routine. Just 30 minutes of exercise in most days of the week is enough to reduce the risk. Healthy body weight is a key to physical and mental wellbeing as obesity increases the risk of breast, cervical, ovarian, and endometrial cancers. Regular physical activity, a healthy diet, and a reduction in the daily intake of calories can help manage weight. Hormone replacement therapy (HRT) can increase the risk of endometrial cancer in women who undergo it after menopause. Women who are seriously considering hormone replacement therapy for their menopausal symptoms should talk to their doctor about the pros and cons of HRT. Hormone replacement therapy may also increase the risk of breast cancer. Bottom line The first thing any woman can do is this: If you experience any of the above-mentioned signs and symptoms of endometrial cancer including pelvic pain, pressure in the lower abdomen or pelvis; unusual vaginal discharge; blood in urine, and pain during intercourse, then make an appointment with your doctor. Endometrial cancer is often detected at an early stage because many women after noticing unusual vaginal bleeding tend to see their doctors. If endometrial cancer is discovered early, removing the uterus surgically often cures endometrial cancer. Heal, Therapy, Insight Facebook Twitter Linkedin
Why More Women in India are Diagnosed with Cancer
Why More Women in India are Diagnosed with Cancer Cancer screening in Hyderabad – This is the right time to get screened for cancer By 2020 India would register 1700000 new cancer cases and approximately 800000 deaths due to cancer. The worrying trend is the increasing number of cancer cases among women. ‘One woman dies of cervical cancer every 8 minutes in India,” while, ”For every 2 women newly diagnosed with breast cancer, one woman dies of it in India.” The most common cancers among women in India are breast, cervical and ovarian cancers. Increasing Number of Breast Cancer Cases in Urban India In urban India, breast cancer is more common as 1 in 22 women living in urban areas is likely to develop breast cancer during her lifetime. This increase in numbers is a cause for concern and it can be attributed to the following lifestyle changes – changes in sleep patterns, high stress, poor eating habits, obesity, sedentary lifestyle, early onset of menarche (Early puberty or menstruation), late menopause and increasing maternal age. Risk Factors of Breast Cancer Women with genetic tests results showing gene mutations in the BRCA1 or BRCA2 genes are at increased risk of developing breast and ovarian cancer. Women with Lynch syndrome are at increased risk of developing uterine, breast and ovarian cancers. Common Risk Factors Apart from the known genetic causes, the exact cause of breast cancer is not known – but there are some risk factors including obesity, late marriage, sedentary lifestyle, eating a high-fat diet, having fewer children and inadequate breastfeeding. Nulliparity, having first pregnancy after 30 years and post-menopausal hormone therapy can also increase breast cancer risk. These risk factors could be leading to more cases of breast cancer in urban India. Ovarian cancer is the third most commonly detected cancer in Indian women In almost 60 to 70% of the cases, the diagnosis of ovarian cancer is made in the later stages of cancer (III or IV stage), Therefore, in India, the five-year survival rate for ovarian cancer is very pathetic (only 45%). For women at relatively higher risk, genetic tests are available to screen the risk of developing ovarian cancer. Cervical cancer is more common in rural India as compared to urban India Cervical cancer is one of the most preventable of all cancers – pelvic examination, pap smear and HPV vaccination is the key to the prevention of cervical cancer in India. Ignorance about the availability of HPV vaccination (This vaccination offers protection against cervical and oral cancers caused by HPV) is one of the reasons for its prevalence in rural India. Bottom Line The development of cancer is an intricate process involving several steps – wherein mutated genes act in unison with several other factors – lifestyle and environmental factors. In other words, genetic, environmental and other risk factors can contribute to cancer growth. Lack of Awareness The number one reason for the increasing number of gynaecological cancers in India is the lack of awareness and comprehensive knowledge about all types of gynaecological cancers. Lack of awareness about the screening programs for breast and cervical cancers and avoidance of regular health check-ups – clinical breast examination, PAP smear and pelvic examination are all the other major factors contributing to the increasing number of gynaecological cancers in rapidly urbanizing India. Late Diagnosis of Breast Cancer The next reason is ignoring the warning signs and symptoms. Delay in approaching a specialist doctor – many women may be diagnosed late because of lack of awareness and reluctance to go to doctors. The best way to ensure early detection, diagnosis and Treatment Outcomes You should talk to your gynaecologist or gynaec-oncologist as soon as you experience any signs and symptoms. Your visit to an oncologist becomes necessary if your symptoms are not responding to basic treatment and have lasted for more than two weeks. If you suspect something abnormal then go for cancer screening in Hyderabad, an early diagnosis can lead to better treatment outcomes and drastically improve survival rates. Heal, Therapy, Insight Facebook Twitter Linkedin
Are We Fighting Ovarian Cancer the Right Way
Being a woman Put You at an increased risk of these health conditions.
Surprising Facts about Ovarian Cancer
Surprising Facts about Ovarian Cancer Facts about ovarian cancer: Oncologists and researchers see ovarian cancer as a big challenge to them. Ovarian cancer is a silent killer. It progresses aggressively, either causing less life-threatening symptoms or no symptoms at all. Research Scientists are studying gene pathways, behavior, and functions. They are also studying the disruptions in the normal genetic functions that can lead to cancer. Scientists are gaining deeper insights into how hormonal and genetic factors play a key role in cancer growth. Researchers and scientists are in the process of finding new ways of screening. SCREENING There is no proper screening test to detect ovarian cancer in the early stages. The detection of ovarian cancer in the early stages can make a huge difference to treatment and prognosis. Gene sequence studies and analysis help in evaluating the future risk of ovarian cancer. Proteomics (the study of the pattern of proteins) is gaining momentum to come up with ways of detecting ovarian cancers early. Symptoms Women ignore these symptoms: stomach disturbances, constipation, gas, and bloating. Owing to this, many women think that these symptoms are due to less life-threatening digestive problems. Therefore, a majority of women tend to ignore the warning signs and thus delay consulting an oncologist. Diagnosis of ovarian cancer Functional MRI and PET/CT scans are also being studied to see where they may be best used for ovarian cancer. Only 20% of ovarian cancers are diagnosed before they spread beyond the ovaries. Nearly about 80% of women miss the diagnosis. The five-year survival rate is sluggish due to late diagnosis. Facts about ovarian cancer – Treatment There is a significant advancement in the surgical and chemotherapy-based treatment approaches of ovarian cancer. The biggest challenge is a slow response to chemotherapy. There is a lack of effective second-line therapy for women who experience episodes of remission and relapse. Heal, Therapy, Insight Facebook Twitter Linkedin
Ovarian Cancer Treatment in Hyderabad
Ovarian cancer treatment in Hyderabad: For the majority of ovarian cancer, surgery is the main treatment. The two main goals of surgery are staging and debulking.