Are We Fighting Ovarian Cancer the Right Way
Being a woman Put You at an increased risk of these health conditions.
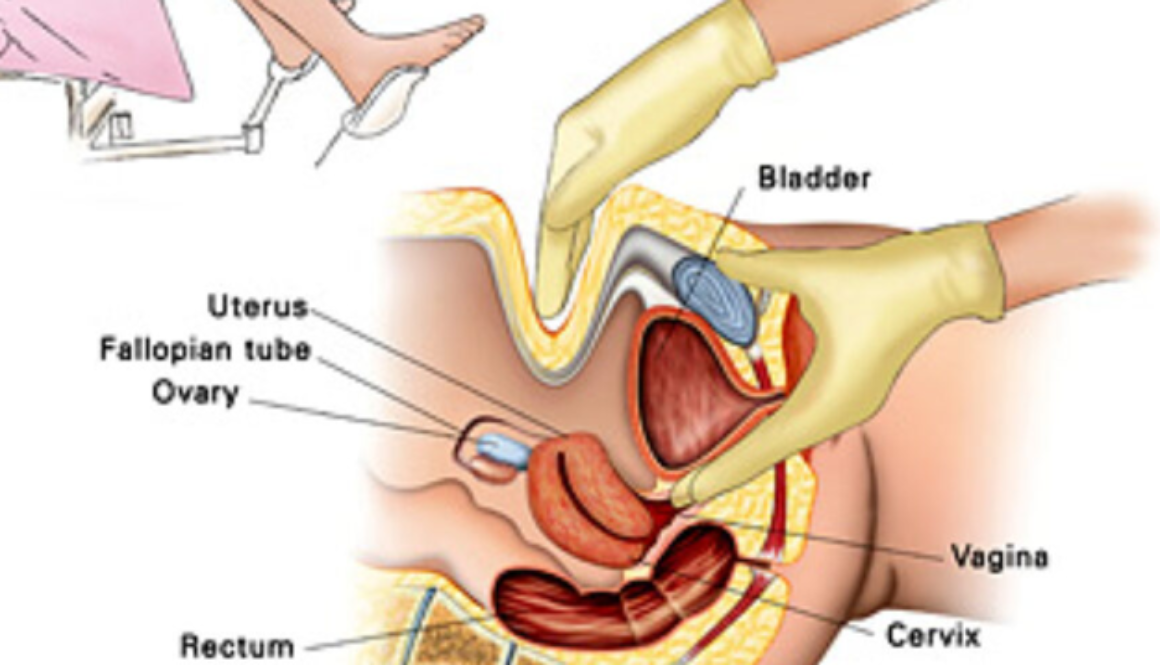
Being a woman Put You at an increased risk of these health conditions.

Take a few minutes to save your life and the life of your loved ones.
Uterine sarcoma is a relatively rare form of cancer that affects the uterus. Though it accounts for only a small percentage of uterine cancers, its impact can be severe. Understanding this type of cancer, its symptoms, risk factors, and treatment options is essential for early detection and improved outcomes.
Uterine sarcoma is a type of malignant tumor that originates in the uterus’s smooth muscle or connective tissue. Unlike more common uterine cancers, which originate in the endometrium (lining of the uterus), uterine sarcoma arises from the supporting tissues of the uterus. The rarity of this cancer makes it challenging to diagnose and treat effectively.
There are several subtypes of uterine sarcoma, each with its own distinct characteristics. The primary types include:
a) Leiomyosarcoma
Among uterine sarcomas, leiomyosarcoma is the prevailing variety. It develops in the myometrium, the muscular layer of the uterus. This aggressive form of cancer tends to grow rapidly and may spread to other parts of the body.
b) Endometrial Stromal Sarcoma
Endometrial stromal sarcoma originates in the connective tissue cells of the endometrium. It is relatively less aggressive compared to leiomyosarcoma and has a better prognosis.
c) Adenosarcoma
Adenosarcoma is a rare type of uterine sarcoma that consists of both benign and malignant components. It usually affects younger women and may present with abnormal vaginal bleeding.
d) Undifferentiated Sarcoma
Undifferentiated sarcoma is a less common type and is characterized by its lack of specific differentiating features. Frequently, it is detected in its later stages, posing challenges for treatment.
The exact cause of uterine sarcoma remains unknown, but certain risk factors may increase the likelihood of its development. These risk factors include:
The symptoms of uterine sarcoma may mimic those of other uterine conditions, making it challenging to diagnose early. Common symptoms include:
If uterine sarcoma is suspected, the following diagnostic tests may be performed:
The treatment for uterine sarcoma depends on various factors, including the type and stage of the cancer, the patient’s overall health, and their preferences. The main treatment modalities include:
a) Surgery
Surgery is the primary treatment for localized uterine sarcoma. The surgeon may perform a hysterectomy, which involves removing the uterus and sometimes surrounding tissues and lymph nodes. For instance, total hysterectomy with salpingo-oophorectomy (the uterus is removed along with one or both ovaries or fallopian tubes)
b) Radiation Therapy
Radiation therapy employs high-energy rays to specifically target and eliminate cancer cells.
It may be used before surgery to shrink the tumor or after surgery to reduce the risk of recurrence. Radiation therapy can be both internal and external.
c) Chemotherapy
Chemotherapy involves using powerful medications to kill cancer cells or stop their growth. It may be used in advanced stages of uterine sarcoma or when the cancer has spread to other parts of the body.
d) Hormone Therapy
Hormone therapy is used for low-grade endometrial stromal sarcoma, as this type of cancer may respond to hormonal treatments.
Q1: What are the survival rates for uterine sarcoma?
The survival rates for uterine sarcoma vary depending on the stage at which it is diagnosed and the type of sarcoma. Generally, early detection and treatment lead to better outcomes. However, the overall five-year survival rate for uterine sarcoma is around 50%.
Q2: Can uterine sarcoma be prevented?
There are no specific measures to prevent uterine sarcoma completely. However, regular gynecological check-ups and reporting any unusual symptoms to a healthcare professional can aid in early detection and better treatment outcomes.
Q3: How is uterine sarcoma different from endometrial cancer?
Uterine sarcoma and endometrial cancer are two distinct types of uterine cancers. Uterine sarcoma arises from the supporting tissues of the uterus, while endometrial cancer originates in the endometrium (lining of the uterus). The treatment approaches and prognosis for these two cancers differ significantly.
Uterine sarcoma is a rare yet critical form of cancer that affects the uterus. Detecting cancer in its early stages and providing suitable treatment is vital for enhancing patient outcomes. If you or someone you know experiences any symptoms related to uterine sarcoma, consult an oncologist. Regular check-ups and awareness are essential to combat this disease effectively.

Gestational Trophoblastic Disease (GTD) is a rare but potentially serious condition during pregnancy. It arises from the abnormal growth of trophoblastic cells, which are responsible for the formation of the placenta. GTD encompasses a range of conditions, including hydatidiform mole, choriocarcinoma, placental site trophoblastic tumor, and epithelioid trophoblastic tumor. Let us delve into the various aspects of GTD, from its symptoms and diagnosis to treatment options and more.
Understanding, Symptoms, and Treatment Options…
Gestational Trophoblastic Disease (GTD) is a group of pregnancy-related disorders characterized by the abnormal growth of trophoblastic cells. These cells usually develop into the placenta during pregnancy. GTD includes hydatidiform mole, which is the most common form, as well as other rare conditions like choriocarcinoma and trophoblastic tumors.
GTD can manifest with a variety of symptoms, which may include:
To diagnose GTD, healthcare providers rely on a combination of methods, including:
The treatment approach for GTD depends on the specific type and extent of the disease:
Certain factors may increase the risk of developing GTD, including:
Q: Can GTD be detected during routine prenatal care?
A: Yes, specific diagnostic tests can detect GTD during routine prenatal care, such as ultrasound imaging and hCG level monitoring.
Q: Is GTD a type of cancer?
A: GTD includes both non-cancerous (hydatidiform mole) and cancerous (choriocarcinoma) conditions, with varying degrees of malignancy.
Q: Can GTD affect future pregnancies?
A: In most cases, women who have had GTD can go on to have successful pregnancies, although close monitoring is essential.
Q: Are there any preventive measures against GTD?
A: Unfortunately, GTD cannot be prevented, but early detection and appropriate treatment can lead to successful outcomes.
Q: Is GTD curable?
A: Yes, the majority of GTD cases are curable, especially when detected and treated early.
Q: How often should follow-up appointments be scheduled after GTD treatment?
A: Regular follow-up appointments are crucial for monitoring hCG levels and ensuring that there is no recurrence of the disease.
Gestational Trophoblastic Disease (GTD) is a complex condition that demands timely detection and proper management. While it can be a source of concern for pregnant individuals, advancements in medical science have led to effective treatment options and positive outcomes. If you suspect any symptoms related to GTD, it’s vital to consult a gynecologic oncologist promptly. Remember, early intervention can make a significant difference in the outcome of the disease.

Post menopausal bleeding
Menopause is a natural biological process that marks the end of a woman’s reproductive years. During menopause, the ovaries gradually decrease their production of estrogen and progesterone hormones, leading to the cessation of menstrual periods. While most women experience menopause between the ages of 45 and 55, it is essential to be aware of certain symptoms that may arise after menopause, such as post-menopausal bleeding (PMB).
Before delving into this condition, let’s first understand menopause itself. Menopause is officially diagnosed after a woman has gone without a menstrual period for 12 consecutive months. It is a natural milestone, but the transitional period leading up to menopause, known as perimenopause, can bring about various physical and emotional changes due to hormonal fluctuations.
During perimenopause, menstrual cycles may become irregular, and women might experience symptoms like hot flashes, night sweats, mood swings, and vaginal dryness. As a woman progresses through perimenopause and into menopause, her ovaries produce fewer hormones, and eventually, menstruation ceases altogether.
Post-menopausal bleeding refers to any vaginal bleeding that occurs twelve months or more after a woman has reached menopause. Since menopause marks the end of the menstrual cycle, any bleeding that happens beyond this point is considered abnormal and requires medical attention.
While PMB can be a result of various benign conditions, it can also be a sign of more serious issues such as endometrial cancer. Therefore, any instance of post-menopausal bleeding should be evaluated promptly by a healthcare professional.
There are several potential causes of post-menopausal bleeding, ranging from harmless to more concerning conditions. Let’s explore some of the common causes:
In some cases, hormonal imbalances can lead to sporadic shedding of the uterine lining, causing post-menopausal bleeding. Fluctuations in estrogen levels can be triggered by factors like stress, weight changes, or certain medications.
As women age and estrogen levels decline, the tissues of the uterus may become thin and fragile, leading to bleeding.
This condition involves an overgrowth of the uterine lining, which can result in irregular bleeding. While hyperplasia itself is not cancerous, certain types can progress to cancer if left untreated.
These are growths that develop in the lining of the uterus. While often benign, they can cause bleeding or other symptoms.
Fibroids are non-cancerous tumors that grow in or on the uterus. While they are common and usually harmless, they can occasionally lead to PMB.
In some cases, post-menopausal bleeding may indicate endometrial cancer, which is cancer that starts in the lining of the uterus.
These are small growths on the cervix that may cause bleeding.
The thinning and drying of the vaginal walls, common after menopause, can lead to bleeding, especially after sexual intercourse.
It’s essential to be aware of the signs and symptoms of post-menopausal bleeding; while bleeding is the primary symptom, other indicators may include:
Vaginal discharge
Pelvic pain or discomfort
Pain during sexual intercourse
Anemia (due to blood loss)
Any episode of bleeding should be reported to a healthcare professional for evaluation.
If you experience abnormal bleeding, it’s crucial not to ignore it. While it may have a benign cause, it could also indicate a more serious underlying issue. To rule out any severe conditions, you should seek medical attention promptly.
Diagnosing the cause of the condition involves a comprehensive evaluation by a healthcare provider. Some common diagnostic methods include:
The doctor will inquire about your medical history, menstrual history, and any other relevant information. A physical examination will also be conducted.
This imaging technique uses sound waves to create images of the pelvic organs, helping to detect any abnormalities in the uterus or ovaries.
A small sample of the uterine lining is collected and examined for any abnormal cells or signs of cancer.
This procedure involves inserting a thin, lighted tube into the uterus to examine the uterine lining closely.
In certain cases, imaging tests like MRI or CT scans may be required to get a more detailed view of the pelvic organs.
Blood tests may be conducted to check for hormonal imbalances or signs of anemia.
The appropriate treatment for post-menopausal bleeding depends on the underlying cause. Some common treatment options include:
Hormone replacement therapy may be prescribed to regulate hormonal imbalances and control bleeding.
During a D&C procedure, the uterine lining is scraped to remove any abnormal tissue.
A hysteroscopy is combined with a D&C to visualize the uterine lining and remove any abnormal growths or tissues.
This procedure involves the destruction of the uterine lining, which can be effective in managing PMB.
In severe cases or if endometrial cancer is detected, a hysterectomy (removal of the uterus) may be recommended.
While post-menopausal bleeding can be caused by cancer, it is essential to remember that many cases are due to benign conditions that can be effectively treated.
You should seek medical attention promptly to determine the cause and appropriate treatment.
Maintaining a healthy lifestyle, including regular exercise, a balanced diet, and stress management, may contribute to overall well-being, but it may not prevent all instances of bleeding.
Hormone therapy may carry some risks, including a potential increase in the risk of certain cancers. It’s crucial to discuss the benefits and risks with your healthcare provider.
Yes, the condition is often treatable, especially when detected early and appropriately evaluated by a healthcare professional.
Post-menopausal bleeding is a concerning symptom that should never be ignored. While the condition can be caused by various factors, it’s crucial to seek medical evaluation promptly to rule out any serious conditions like endometrial cancer. Early detection and appropriate treatment can significantly improve outcomes and overall well-being. Remember, regular check-ups and open communication with your gynecologist are essential to maintaining optimal health during and after menopause.
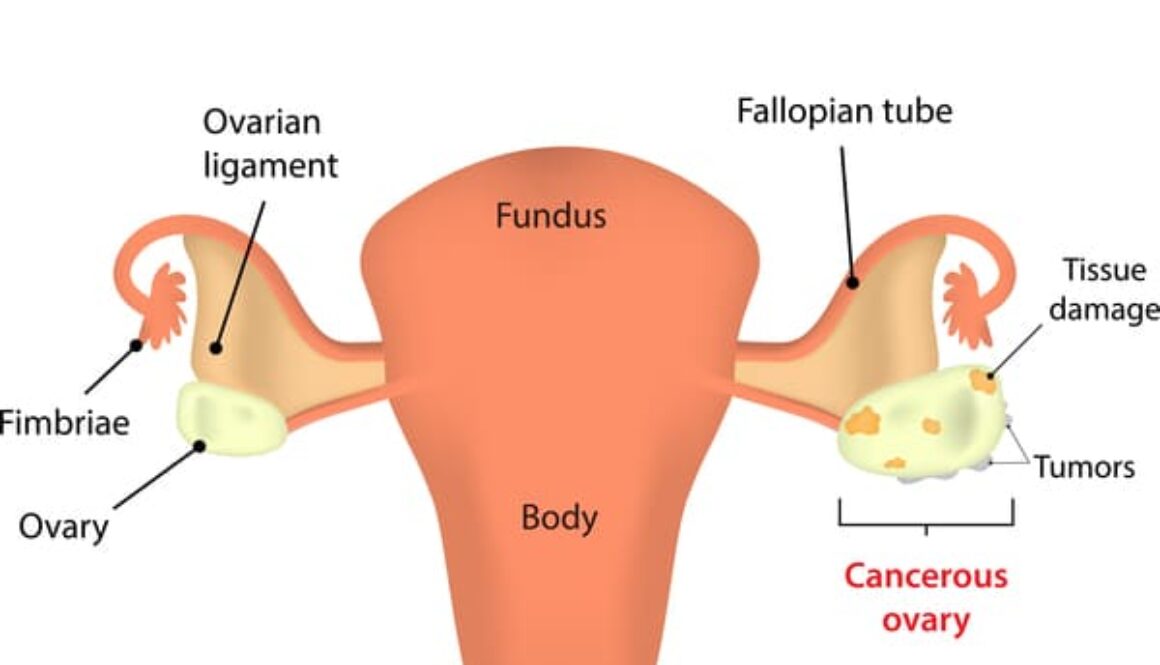
Ovarian Cancer Screening
Ovarian cancer is a disease that has the potential to be life-threatening and impacts numerous women around the globe. Early detection and timely intervention play a crucial role in improving the prognosis and survival rates of ovarian cancer patients. In this article, we will delve into the topic of ovarian cancer screening, exploring its importance, methods, and considerations. By understanding the available screening options, women can make informed decisions about their health and take proactive steps toward early detection.
What is Ovarian Cancer?
Ovarian cancer is a type of cancer that originates in the ovaries, the reproductive organs responsible for producing eggs. It occurs when abnormal cells in the ovaries grow and divide uncontrollably, forming tumors. Ovarian cancer can spread to nearby organs and, if left untreated, metastasize to distant sites in the body.
The exact cause of ovarian cancer remains unknown, but certain risk factors have been identified. These include a family history of ovarian or breast cancer, inherited gene mutations (such as BRCA1 and BRCA2), increasing age, hormone replacement therapy, and obesity. However, it’s important to note that having one or more risk factors doesn’t guarantee the development of ovarian cancer.
Ovarian cancer often presents with nonspecific symptoms in its early stages, making it challenging to diagnose. By undergoing regular screening tests, women have a better chance of detecting ovarian cancer at an early, more treatable stage. Early detection significantly improves the prognosis and increases the chances of successful treatment.
Certain individuals have a higher risk of developing ovarian cancer and may benefit from proactive screening. High-risk groups include women with a family history of ovarian or breast cancer, those with known gene mutations (BRCA1 and BRCA2), and individuals who have previously had breast, ovarian, or colorectal cancer.
Transvaginal ultrasound is a commonly used screening method for ovarian cancer. It involves inserting a small ultrasound probe into the vagina to obtain images of the ovaries. This non-invasive procedure helps identify any abnormal growths or cysts that may require further investigation.
The CA-125 blood test is utilized to determine the concentration of a protein known as CA-125 in the bloodstream. Elevated CA-125 levels can indicate the presence of ovarian cancer, although it is not specific to this disease. This test is often used in conjunction with other screening methods to improve accuracy.
For individuals with a family history of ovarian or breast cancer, genetic testing can provide valuable insights into their risk of developing ovarian cancer. Individuals can make informed decisions about screening and preventive measures by identifying specific gene mutations, such as BRCA1 and BRCA2.
The age at which ovarian cancer screening should begin and the frequency of screening depend on various factors, including personal and family history. In general, most guidelines recommend starting regular screening around the age of 40 or 50 and continuing until the age of 75, unless other risk factors are present.
For women at high risk due to family history or genetic mutations, screening may be recommended at an earlier age and conducted more frequently. Healthcare providers will assess individual risk factors and tailor screening recommendations accordingly.
Screening tests have the potential to detect ovarian cancer at an early stage when treatment options are more effective. Early detection can lead to better outcomes and improved survival rates. Regular screening may also identify benign conditions or non-cancerous cysts, providing reassurance to individuals.
Ovarian cancer screening can sometimes produce false-positive results, indicating the presence of cancer when none is actually present. False-positive results can cause anxiety and may lead to unnecessary
invasive procedures or surgeries. It’s important for individuals to discuss the benefits and limitations of screening with their healthcare providers.
Personal and Family History
Individuals with a family history of ovarian or breast cancer are at higher risk and should consider discussing screening options with their healthcare providers. They may be referred to genetic counseling or offered genetic testing to determine their individual risk profile.
Genetic Predisposition
Known genetic mutations, such as BRCA1 and BRCA2, significantly increase the risk of developing ovarian cancer. Individuals with these mutations should consider proactive screening and explore risk-reducing options such as prophylactic surgeries.
Surgical Interventions
Some individuals may have undergone surgical procedures, such as tubal ligation or hysterectomy, which reduce the risk of ovarian cancer. However, it’s important to note that these procedures do not eliminate the risk entirely, and screening may still be recommended based on individual circumstances.
Discussing Screening Options
Women should have open and honest discussions with their healthcare providers about their individual risk factors, concerns, and preferences regarding ovarian cancer screening. Healthcare providers can guide patients through the available options and help them make informed decisions.
Shared Decision-Making
Shared decision-making is a collaborative process between patients and healthcare providers to determine the best course of action based on individual circumstances. This approach ensures that patients are actively involved in their healthcare decisions and have a thorough understanding of the benefits and potential risks of screening.
Maintaining a healthy lifestyle can help reduce the risk of ovarian cancer. Engaging in regular physical activity, maintaining a balanced diet rich in fruits and vegetables, and avoiding tobacco use can contribute to overall well-being and lower the risk of developing various cancers, including ovarian cancer.
Studies have shown that the use of oral contraceptives (birth control pills) can reduce the risk of ovarian cancer. Women should discuss the potential benefits and risks of oral contraceptives with their healthcare providers to determine the most suitable options for them.
For individuals at high risk of ovarian cancer, risk-reducing surgeries such as bilateral salpingo-oophorectomy (removal of the ovaries and fallopian tubes) may be considered. These surgeries significantly reduce the risk of developing ovarian cancer but should be carefully discussed with healthcare providers due to their potential impact on fertility and hormonal balance.
Ovarian cancer screening is a vital component of women’s healthcare, offering the opportunity for early detection and improved outcomes. By understanding the available screening methods, guidelines, and considerations, women can actively participate in their health decisions and take the necessary steps to protect themselves. Consult with your healthcare provider to assess your risk factors, discuss screening options, and determine the best approach for your individual circumstances.
No, ovarian cancer screening is not 100% accurate. While screening tests can help detect potential abnormalities, they can also produce false-positive or false-negative results. It’s important to discuss the benefits and limitations of screening with your healthcare provider.
Ovarian cancer often presents with vague symptoms that may resemble other less severe conditions. These symptoms may include abdominal bloating, pelvic pain, frequent urination, and changes in bowel habits. If you experience persistent or worsening symptoms, consult your healthcare provider for evaluation.
While ovarian cancer cannot be entirely prevented, certain risk-reducing strategies can lower the chances of developing the disease. Lifestyle modifications, oral contraceptives, and risk-reducing surgeries may be considered based on individual circumstances and risk factors.
Learn more about – Cancer Prevention – Is It Possible?
Transvaginal ultrasound and the CA-125 blood test are the most commonly used screening methods for ovarian cancer. Alternative methods, such as pelvic exams or tumor markers, have limited effectiveness as standalone screening tools.
The frequency of ovarian cancer screening depends on individual factors, including age, family history, and genetic predisposition. It’s essential to discuss screening guidelines and recommendations with your healthcare provider to determine the most suitable screening interval for you.
Learn more about Ovarian Cancer
Cancer is a formidable disease that affects millions of women worldwide. Detecting cancer in its early stages is crucial for successful treatment and improved survival rates. By identifying cancer before it spreads to other parts of the body, medical professionals can employ targeted interventions that have a higher likelihood of success.
Early detection of cancer in women plays a crucial role in saving lives and improving treatment outcomes. By identifying cancer at its initial stages, medical professionals can provide timely interventions and improve the chances of successful treatment. In this article, we will explore the importance of early detection, discuss common screening methods, and highlight the key steps women can take to proactively detect cancer.
Early detection of cancer allows for more treatment options and can significantly increase the chances of a positive outcome. It enables medical professionals to intervene before the disease progresses, leading to better treatment responses and improved quality of life for patients.
Early diagnosis of cancer provides several benefits. It can lead to less aggressive treatment interventions, reducing the potential for complications. Additionally, it offers peace of mind to individuals who receive timely medical attention and helps alleviate anxiety associated with uncertainties regarding their health.
Several types of cancer are prevalent in women. It is essential to understand these cancers to recognize their symptoms and seek appropriate medical attention promptly. The following are some of the most common types of cancer that affect women:
Breast cancer is one of the most common types of cancer among women. Regular mammograms and self-examinations are key in detecting breast cancer at an early stage when treatment options are most effective.
Cervical cancer affects the cervix, the lower part of the uterus. Regular Pap tests, which involve screening for abnormal cells in the cervix, are crucial for early detection and successful treatment.
Ovarian cancer occurs in the ovaries and is often challenging to detect in its early stages. However, routine pelvic exams and awareness of potential symptoms can contribute to early detection.
Colorectal cancer affects the colon or rectum and can be detected through regular colonoscopies. Early detection can improve survival rates and increase treatment options.
Screening methods play a vital role in the early detection of cancer. The following are common screening techniques used for detecting cancer in women:
Mammograms are X-ray images of the breasts that can detect abnormalities, including lumps or tumors. Women are encouraged to undergo regular mammograms, especially as they age.
Pap tests involve collecting cells from the cervix and examining them for any abnormalities. Women should receive regular Pap tests as part of their routine healthcare.
During pelvic exams, healthcare professionals examine the pelvic region for any signs of abnormality, including ovarian masses or growths. Regular pelvic exams are essential for detecting potential ovarian cancer.
Colonoscopies are procedures that examine the colon and rectum for abnormalities. They can help detect polyps or early signs of colorectal cancer. Regular colonoscopies are recommended for individuals at risk.
Understanding the risk factors associated with cancer in women is essential for prevention and early detection. While some factors, such as genetics, cannot be changed, adopting healthy lifestyle choices and regular screenings can significantly reduce the risk. Key prevention strategies include:
Some women may have a genetic predisposition to certain types of cancer, such as breast or ovarian cancer. Understanding family history and considering genetic testing can help identify individuals at higher risk.
Maintaining a healthy lifestyle can contribute to overall well-being and lower the risk of cancer. Engaging in regular physical activity, following a balanced diet, limiting alcohol consumption, and avoiding tobacco products are important preventive measures.
Women should prioritize regular check-ups and self-examinations to detect any changes or abnormalities in their bodies. Being proactive and alert to potential symptoms can lead to early detection and timely medical intervention.
Raising awareness about early detection and cancer prevention is crucial to saving lives. Public health campaigns, community outreach programs, and educational resources play a vital role in empowering women with knowledge and promoting regular screenings. Support groups and online resources can also provide valuable information and support to those affected by cancer.
Early detection of cancer in women is a vital component of effective treatment and improved outcomes. By understanding the importance of early diagnosis, familiarizing themselves with common screening methods, and adopting preventive strategies, women can take proactive steps to safeguard their health. Regular screenings, self-examinations, and maintaining a healthy lifestyle can significantly contribute to the early detection and successful treatment of cancer.
At what age should women start getting regular mammograms?
Answer: Women should discuss with their healthcare providers when to start regular mammograms, as recommendations may vary based on individual risk factors and guidelines.
It is generally recommended that women start getting Pap tests at the age of 21 and continue with regular screenings every three years, or as advised by their healthcare provider.
Answer: Ovarian cancer often presents with subtle or nonspecific symptoms, such as bloating, abdominal pain, changes in bowel habits, or urinary urgency. It is important to consult a healthcare professional if these symptoms persist.
While not all cases of colorectal cancer can be prevented, adopting a healthy lifestyle, including a balanced diet rich in fruits and vegetables, regular physical activity, and avoiding smoking and excessive alcohol consumption, can help reduce the risk.
There are numerous organizations, support groups, and online resources dedicated to providing information and support to individuals affected by cancer. Your healthcare provider can also provide guidance and direct you to appropriate resources.
In conclusion, early detection of cancer in women is vital for effective treatment and improved outcomes. By being proactive, following recommended screening guidelines, and adopting healthy lifestyle choices, women can take charge of their health and increase their chances of detecting cancer at its earliest and most treatable stage. Stay informed, prioritize regular check-ups, and spread awareness about the importance of early detection to protect the well-being of women everywhere.

Breast cancer is a complex disease that requires a comprehensive treatment plan tailored to the individual needs of each patient. With advancements in medical science, there are now various treatment options available to effectively manage breast cancer and improve the chances of survival. This article explores the different aspects of a treatment plan for breast cancer, including its definition, understanding the disease, treatment options, creating a personalized approach, potential side effects, and coping mechanisms.
Breast cancer is a type of cancer that develops in the cells of the breasts. It is the most common cancer among women globally, affecting millions of lives every year. A well-structured treatment plan is crucial in combating breast cancer and ensuring the best possible outcome for patients. This article aims to provide insights into developing a treatment plan that addresses the unique needs and circumstances of individuals diagnosed with breast cancer.
Breast cancer is characterized by the abnormal growth of cells in the breast tissues. There are several types of breast cancer, including ductal carcinoma in situ (DCIS), invasive ductal carcinoma, invasive lobular carcinoma, and inflammatory breast cancer. Understanding the specific type and stage of breast cancer is essential in determining the most appropriate treatment approach.
While the exact causes of breast cancer remain unknown, certain risk factors have been identified. These include a family history of breast cancer, genetic mutations (such as BRCA1 and BRCA2), hormonal factors, age, lifestyle choices, and exposure to radiation or certain chemicals. It is crucial to assess these risk factors to develop an effective treatment plan.
Breast cancer may present various symptoms, such as a lump or thickening in the breast or underarm area, changes in breast size or shape, nipple changes, skin dimpling, or nipple discharge. Prompt diagnosis is essential for timely treatment. Diagnostic procedures such as mammograms, ultrasounds, biopsies, and MRI scans help determine the presence and extent of breast cancer.
A multidisciplinary approach combining different treatment modalities is often employed in the management of breast cancer. The following are the primary treatment options used:
Surgery plays a crucial role in the treatment of breast cancer. The two main surgical procedures are:
Lumpectomy, also known as breast-conserving surgery, involves removing the tumor and a small portion of surrounding healthy tissue. This procedure aims to preserve the breast while effectively treating cancer.
A mastectomy is a surgical procedure that involves the complete elimination of breast tissue. It may be recommended in cases where the tumor is large or has spread to other parts of the breast. Depending on the individual’s situation, reconstructive surgery can be performed after mastectomy.
Radiation therapy utilizes high-energy X-rays or other particles to eliminate cancer cells. It is commonly used after surgery to eliminate any remaining cancer cells and reduce the risk of recurrence.
Chemotherapy utilizes powerful drugs to destroy cancer cells throughout the body. It can be administered before surgery (neoadjuvant chemotherapy) to shrink tumors, after surgery (adjuvant chemotherapy) to eliminate any remaining cancer cells, or as the primary treatment for advanced or metastatic breast cancer.
Hormone therapy is typically recommended for hormone receptor-positive breast cancers. It aims to block the effects of hormones like estrogen or progesterone, which can fuel the growth of certain breast cancer cells. Hormone therapy may include medications like tamoxifen, aromatase inhibitors, or ovarian suppression.
Targeted therapy involves drugs specifically designed to target and block the growth of cancer cells. These medications, such as trastuzumab, pertuzumab, or lapatinib, are commonly used for HER2-positive breast cancers.
Developing a treatment plan for breast cancer involves collaboration between a medical team, including oncologists, surgeons, radiologists, and other specialists. Here are some key considerations in creating an effective treatment plan:
Building a strong medical team that specializes in breast cancer treatment is vital. This team should include healthcare professionals who can provide guidance, support, and expertise throughout the treatment journey.
Each breast cancer case is unique, and treatment plans should be personalized to address the individual’s specific circumstances. Factors such as cancer stage, type, genetic makeup, overall health, and personal preferences should be taken into account.
When determining the best treatment plan, factors such as potential benefits and risks of each treatment modality, possible side effects, long-term implications, and the individual’s emotional well-being should be carefully considered.
Breast cancer treatments may cause various side effects that can impact the patient’s quality of life. These can include fatigue, hair loss, nausea, weight changes, fertility issues, menopausal symptoms, and emotional distress. It is important for patients to be aware of these potential side effects and work closely with their medical team to manage them effectively.
A breast cancer diagnosis can be emotionally challenging. It is crucial to develop coping mechanisms and seek support from healthcare professionals, support groups, friends, and family. Engaging in self-care activities, maintaining a healthy lifestyle, and staying informed about the latest research and advancements can empower individuals in their journey toward recovery.
A well-structured treatment plan for breast cancer is essential in effectively managing breast cancer and improving patient outcomes. By understanding the different treatment options available, working closely with a medical team, and considering individual circumstances, patients can navigate their breast cancer journey with confidence. Regular screenings, early detection, and a proactive approach to treatment can significantly increase the chances of successful outcomes.
Breast cancer treatment duration varies depending on factors such as cancer stage, treatment modalities, and individual response. It can span from a few months to several years.
Certain treatments, such as chemotherapy, may impact fertility temporarily or permanently. It is important to discuss fertility preservation options with your healthcare team before starting treatment.
While complementary therapies can help manage side effects and improve well-being, they should not replace conventional medical treatments. It is crucial to consult with your medical team before incorporating any alternative therapies.
Genetic testing helps identify genetic mutations that may increase the risk of breast cancer. This information can guide treatment decisions and help determine the need for preventive measures in family members.
The frequency of follow-up appointments may differ based on individual circumstances. Generally, regular follow-up visits are recommended to monitor recovery, address any concerns, and detect any potential recurrence or new developments. If you have any queries regarding any other treatment modality for breast cancer, then meet Dr. Geetha Nagasree at Care Hospitals, Gachibowli, Hyderabad

How to prevent gynecologic cancer – Dr. Geetha Explains
Gynecological cancers refer to cancers that affect the reproductive organs of women, including the cervix, ovaries, uterus, fallopian tubes, vagina, and vulva. While certain risk factors like age, genetics, and family history cannot be controlled, there are steps that women can take to lower their risk of developing gynecological cancers.
Get regular screenings: Regular screenings for cervical, ovarian, and other gynecological cancers can help detect cancer early when they are most treatable. Talk to your healthcare provider about when to start getting screened and how often to do it.
Practice safe sex: Practicing safe sex and getting vaccinated against the human papillomavirus (HPV) can reduce your risk of cervical and vaginal cancers. Cervical cancer – the main cause is often a sexually transmitted virus: HPV. It often leads to cervical cancer in women.
Maintain a healthy weight: Being overweight or obese increases the risk of endometrial and ovarian cancers. Eating a healthy diet and exercising regularly can help you maintain a healthy weight and lower your cancer risk.
Quit smoking: Smoking increases the risk of several types of cancer, including cervical and vaginal cancers. Smokers are 3 to 4 times at increased risk compared to non-smokers. If you smoke, talk to your general physician regarding the ways to quit smoking.
Limit alcohol consumption: Drinking alcohol in excess can increase the risk of several types of cancer, including breast, ovarian, and endometrial cancers. If you choose to drink, do so in moderation.
Be aware of your family history: Some gynecological cancers can run in families. If you have a family history of gynecological cancers, talk to your healthcare provider about ways to reduce your risk.
Practice good hygiene: Practicing good hygiene can help reduce the risk of vulvar cancer. This includes keeping the genital area clean and dry, wearing cotton underwear, and avoiding scented and chemical-based products.
By following these steps, women can reduce their risk of developing gynecological cancers and maintain their overall health and well-being.
If you still have concerns regarding how to prevent gynecologic cancer, then
Dr. Geetha Nagasree recommends adopting the following healthy habits to lower your risk of gynecologic cancer:
Vaccinate against HPV: If you’re between 9 and 45 years old, getting vaccinated against HPV can protect you from the types of HPV that commonly cause cervical, vaginal, and vulvar cancers. Talk to your healthcare provider about when you or a family member should get the HPV vaccine.
To ensure early detection and reduce the risk of cervical cancer, it’s essential to schedule regular Pap tests. Dr. Geetha highly recommends undergoing Pap tests regularly, even if you’ve received an HPV vaccine. A Pap test examines the cells in your cervix to detect any abnormalities that could develop into cancer. It’s important to note that if you were assigned female at birth, regardless of your gender identity, you likely have a cervix.
To reduce the risk of gynecologic cancer, it’s essential to adopt healthy habits. While screening for cervical cancer is available, there are currently no simple, reliable tests for other types of gynecologic cancer. Therefore, it’s crucial to pay attention to any symptoms and seek medical advice promptly if you notice any changes.

How to Prevent Cancer in Future | Dr. Geetha Explains
What are some ways individuals can reduce their risk of developing cancer? Despite the abundance of recommendations, sometimes advice from one study contradicts advice from another. Nonetheless, it is widely acknowledged that lifestyle choices can impact the likelihood of developing cancer, although cancer prevention knowledge is still evolving. Let us have a look at some of the ways by which you can prevent cancer.
Tobacco use has been associated with numerous forms of cancer, such as lung, mouth, throat, voice box, pancreas, bladder, cervix, and kidney. Even exposure to secondhand smoke can heighten the risk of lung cancer.
Moreover, chewing tobacco has also been linked to cancer of the mouth, throat, and pancreas. To reduce the likelihood of developing cancer, it’s crucial to refrain from using tobacco or quit using it entirely. Individuals who want to quit smoking can seek assistance from healthcare professionals, who can recommend stop-smoking products and other cessation methods.
Consuming alcohol raises the likelihood of different forms of cancer such as breast cancer, colon cancer, lung cancer, kidney cancer, and liver cancer. The risk of developing cancer is amplified when consuming larger quantities of alcohol. Quitting alcohol altogether or consuming in moderation is the best way to prevent cancer in future.
According to a report from the World Health Organization’s International Agency for Research on Cancer, consuming processed meat on a regular basis can marginally elevate the chances of developing particular forms of cancer.
Construct your diet primarily around fruits, vegetables, and other plant-based foods like whole grains and beans. Make your meals lighter and more nutritious by opting for fewer high-calorie foods. Constrain your intake of refined sugars and animal-derived fats.
Consuming a Mediterranean diet that incorporates mixed nuts and extra-virgin olive oil may lower the possibility of developing breast cancer. The Mediterranean diet prioritizes plant-based foods like fruits, vegetables, whole grains, legumes, and nuts. Those who adhere to this diet prefer healthier fats, such as olive oil, to butter and replace red meat with fish.
Having protection against certain viral infections may assist in safeguarding against cancer. It is recommended to consult with an expert oncologist regarding getting vaccination against these infections.
Having multiple sexual partners, having a sexual partner who is promiscuous, homosexual, and having sexually transmitted infections can all elevate the likelihood of contracting hepatitis B, which in turn can raise the risk of developing liver cancer.
Individuals who are at elevated risk include those who engage in the injection of illicit drugs, men who have sex with other men, and healthcare or public safety personnel who may come into direct contact with infected bodily fluids or blood.
HPV is a virus that can be transmitted through sexual activity. It can cause various types of cancer, such as cervical cancer, genital cancer, and squamous cell cancer in the head and neck region. To prevent HPV infections, vaccination is recommended for both girls and boys at the ages of 11 and 12. The Gardasil 9 vaccine has been approved by the U.S. Food and Drug Administration for use in males and females between the ages of 9 and 45.
Regularly examining oneself and undergoing screenings for various types of cancers such as skin, colon, cervix, and breast cancer can increase the likelihood of detecting cancer early. Early detection leads to an increased probability of successful treatment. Consult Dr. Geetha Nagasree – a renowned oncologist in Hyderabad to determine the best cancer screening schedule for your specific needs.